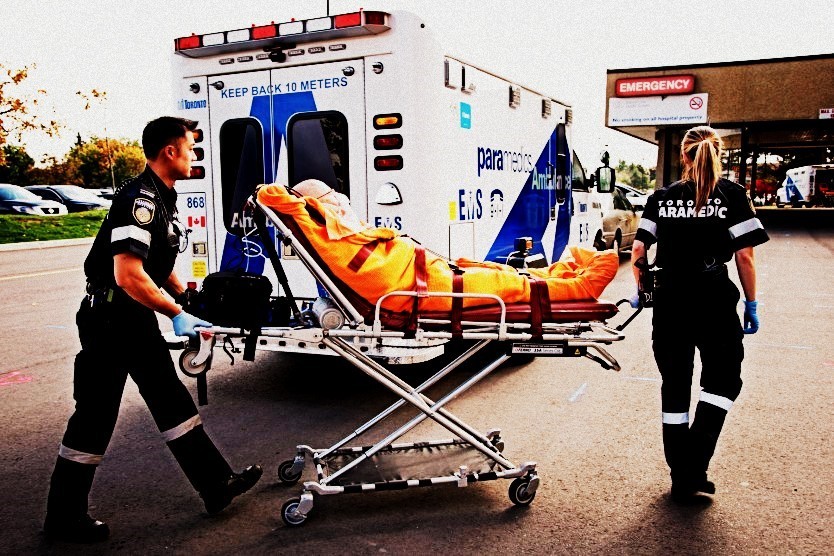
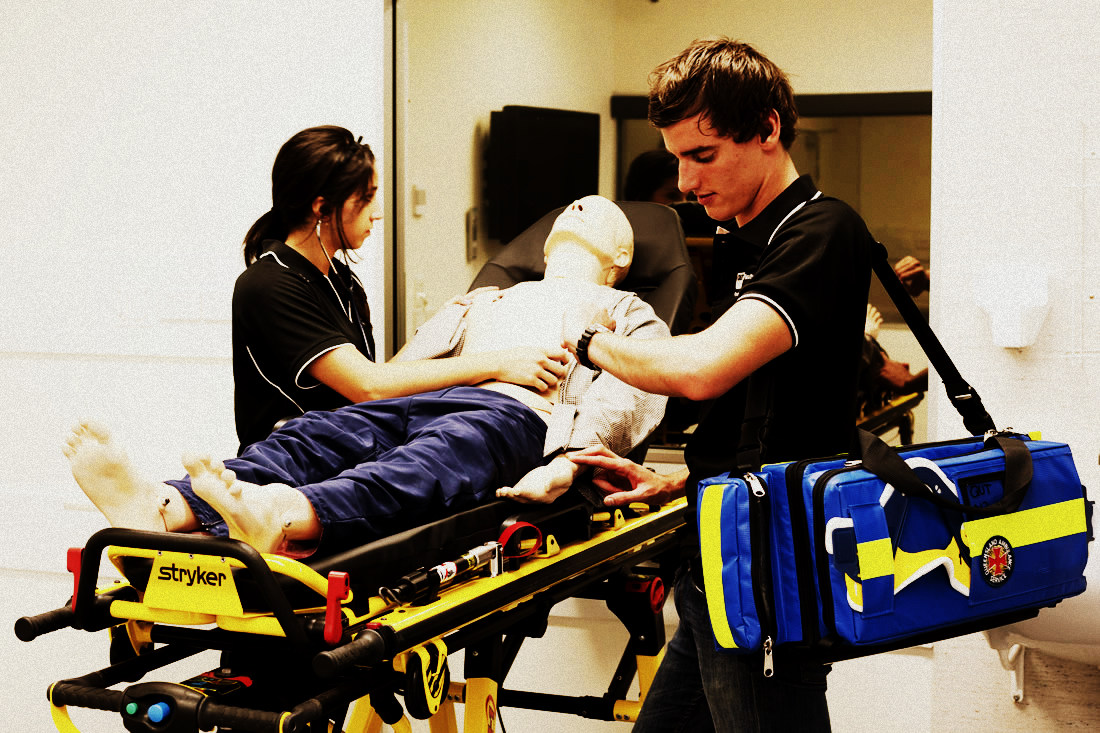
Throughout history, paramedicine has never remain stagnant.
Paramedic duties have intensified over time.”
The transformation of our world has introduced changes and altered many of our norms. Some practices have become outdated, while others remain relevant. For Emergency Medical Service, these norms apply to training, equipment, legal protection, job description, technology, self-care and self-defense, accreditation, wages, and the understanding of subcultures in the community.
Throughout history, paramedicine has never remained stagnant. Paramedic duties have intensified over time. And as such, we should first define Emergency Medical Service and show how this profession has evolved. We can only predict how it may progress beyond the information and technological age. Let’s focus on the psychosocial model of the work.
WHAT IS AN EMERGENCY RESPONDER
According to EMS1.com, Emergency Medical Service (EMS) is provided by a “trained medical professional” who can deliver treatment and transport for people in crisis health situations that may be life-threatening. EMT is an entry-level position in Emergency Medical Service. Once you become an EMT, you can progress to more advanced training, such as a Primary Care Paramedic, Advance Care Paramedic, and Critical Care Paramedic.
Career Bear describes a paramedic as a “first responder, working alongside police and firefighters to provide emergency service and pre-hospital care for patients.” Ottawa Paramedics traced the history of paramedicine back to 900AD and marked it as the oldest service in the world.
The Ontario Paramedic Association gave a timeline that began in 1832 where “due to the demand for help in removing ill and deceased victims during a deadly cholera outbreak in the Town of York (now Toronto), June 22, 1832, saw the establishment of the first organized form of Ambulance transportation”. Emergency Medical Service is an age-old profession.
Throughout history, every modification was due to necessity. Ontario Paramedics also charted 1930s to 1960s as the pinnacle moment for EMS in Ontario.”
After establishing organized Ambulance transportation n in Canada, further incidents led to several turning points that caused the expansion of emergency first response in the country. Whether it was in 1880 when “formalized Hospital based Ambulance service began in Toronto with the Toronto General Hospital taking delivery of what is believed to be Canada’s first horse-drawn Ambulance” or twenty-five years later in 1905 when “independent entrepreneurs became Private Ambulance providers until control of Ambulance services fell under the jurisdiction of the Provincial government.”
Throughout history, every modification was due to necessity. Ontario Paramedics also charted the 1930s to 1960s as the pinnacle moment for EMS in Ontario. “These years also saw the addition of the NGOs in Ambulance and disaster service. Organizations like The St. John Ambulance Brigade and the Canadian Red Cross added staff and vehicles to assist in treating and transporting the ill and injured. In addition to the many new and developing ambulance services, training was also adapting to the need of the time.”
Legal protection, street smart, self-defence, the ability to maneuver complex technological gadgets.”
In 1977, about seventy-two years after Ambulance services fell under the provincial government’s jurisdiction, Dr. Norman H. McNally, revered as “The “Father” of Ontario’s modern-day EMS system,” died. His vision for advanced paramedic training and aero-medical transportation of patients in Ontario was soon realized. In 1995 “the next major step in Ontario came from preliminary OPALS results.
EMS has continually grown. All Ontario ambulance staff were trained to defibrillate patients in cardiac arrest. Six medications designed to provide “Symptom Relief” for limited emergency medical conditions the following year spread a few Advanced Life Support skills to everyone. By 2008, “the job for someone with a heavy foot, a chauffeur’s license, and a strong back” had evolved from a two-year Community College certificate program to a 2-year University program with Paramedics graduating with a BSc degree.
CULTURAL AWARENESS
With the countenance of cultural awareness, many people immediately assume political activism. They anticipate arguments about racism, discrimination, or even bigotry. They were driving while Black, flying while Arab, mingling while Aboriginal or white supremacy is the least of our social issues anymore. Legal protection, street smart, self-defense, the ability to maneuver complex technological gadgets, to understand, communicate and gain the trust of people outside of a medic’s professional environment are the way of the future for Emergency Responders.
Since medics are not police, they do not have the stigma associated with law enforcement. EMS does not give citations, arrests, kills, or summons, so they do not envy. However, one would expect everyone in the community to cooperate with them, but you would be amazed to see differences.
On September 11, 2001, majority of the casualties were first responders and firefighters.”
Terrorism has a direct effect on paramedicine. Cultural awareness suggests a realization that there are enormous undetermined risks for all first responders, especially with the spread of conspiracy theories. Is the government conditioning the public? Are EMS workers a systemic go-between who subtly infringe on constitutional freedoms? Etc. Meanwhile, critical aspects of 1) national security, 2) street and prescription drug overindulgence, and 3) the craze in some trendy subcultures may disturb an EMS worker in the field.
Emergency Medical Service needs mental preparation to provide effective uninterrupted care, especially after an attack. Our society has realized that some people wish to inflict harm on us. This does not only elude to sound education, reasonably, but it is also about legal protection against physical attack while administering treatment in the field. On September 11, 2001, most of the casualties were first responders and firefighters.
Also, first responders ought to be prepared to protect their rights and personal safety. By this, I’m not referring to weight lifting or exercises though they are essential. I’m not referring to a psychological resilience to gruesome scenes or an emotional fortitude. These are all admirable traits, but I’m referring to wit, legal protection against potential lawsuits, the availability of cutting-edge equipment and training on utilizing them in the public’s eye, hazard drills, and social awareness of cultural orientations which may have negative stereotypes.
Emergency Responders should know cultural and religious norms in Black, Brown, Aboriginal, and other White communities. Through this understanding, there can be a different pattern of behavior. This is key when avoiding lawsuits or complaints stemming from biases, discernment, preconceptions, or a simple mistrust of a stranger due to stereotypes.
I presume a time in the near future when medics will need detailed self-defence training.”
Secondly, with public indulgence in the street and prescription drugs, an encounter with someone under the influence can become violent. September 11, 2001, also taught us that sometimes there might not be enough time to pull back.
Violence can vary from a fist-to-fist confrontation and the use of a baseball bat, knife, or machete to that of a firearm or explosive. I presume a time shortly when medics will need detailed self-defense training. As of now, paramedicine is vast in the treatment of drug overdose. Unless better medications were put at the medic’s disposal, the issue I foresee is not how to treat a cooperating patient under the influence. Instead, it is how medics should protect themselves in an unexpected physical attack where someone under the influence of a newer, more potent drug may result in unexpected ferocity.
Medics should be authorized and prepared not only to use sound discretion in the case of a biological or other severely hazardous attack but how to defend should need be. This is patient care in the streets, where anything can happen at anytime.
Thirdly, the growing influence of trendy subcultures can also bring a medic face to face with a delinquent. A medic has to be culturally savvy to Pop and Hip Hop culture, especially in identifying real gangsters from ordinary people who live the lifestyle. Most lifestyles run parallel with the environment the person lives in. A Proper understanding of the biopsychosocial network of a particular subculture can help in de-escalation.
Here are people who quickly judge and spread rumors, yet their judgments are primarily based on ignorance. A subculture may be stigmatized for no good reason. I remember being mistaken for a gangster because I rap and speak Ebonics. The people who mistook me for a gangster did so because they did not understand the inner-city culture. And they believed wholeheartedly that they were right. Can you imagine such a person becoming a police officer or an Emergency Responder? It will be devastating for an average person living outside the system.
You cannot send someone into the streets to perform a trustworthy responsibility when the person is not mindful of the makings of street culture. Not everyone who listens to rap, swears in slang or speaks Ebonics is criminal, unprofessional, or a troublemaker. Real gangsters belong to a real gang to which they have sworn allegiance under oath.
The medic should be aware of street essence in these influential subcultures within the community. That’s being street smart.”
They commit organized crime as part of their illicit business to fund their operation. This differs significantly from someone from the suburbs or the inner city community who has never joined a gang but does not believe the “white way is the right way.” To tell the difference, a medic must be street-smart. Emergency Medical Responders should be able to distinguish gang graffiti and tattoos from none gang graffiti and tattoos. The doctor should know the street essence in these influential subcultures within the community.
That’s being street smart. One cannot simply expect to teach or train people to change who they are or alienate or deprive them of opportunities hoping this will force them to conform; not legitimizing a subculture gives it a cause for continued defiance. A medic may even come from a subculture and identify with it in an encounter with another person from that community.
MODERN UPGRADE OF EQUIPMENT, TRAINING, AND DUTIES
Every generation thinks they’re modernized. For example, the 1920s generation thought they were living in a modern time just because we believe we live in modern times. Indeed if you look at it, you will see that it was only three years ago when in-dash global positioning systems became prevalent. Even at that, our current ambulances are not standardly equipped with GPS. I’m implying that as modern as we think we are, there will always be a more modern time. There are four basic levels of Emergency Responders in Canada, 1) The Emergency Medical Technician, 2) the Primary Cara Paramedic, 3) the Advance care paramedic, and 4) Critical Care Paramedics.
I envision a future in which cultural awareness as it pertains to trendy subcultures
in our community, tomorrow’s version of modern upgrade of equipment.”
Though it is commendable that there are degree programs for paramedic training in some universities in Canada, the growing need for nurses and physicians in an emergency is only going to increase. I believe shortly Emergency Medical Services should be upgraded to the equivalence of Registered Practical Nurses, Registered Nurses, and Nurse Practitioners.
PCP should be an associate degree program. Advanced and Critical Care Paramedics should be in bachelor’s and master’s degree programs with further training and authorization to order tests, interpret them, and prescribe medications. As far-fetched as this might seem, it was only in the 1970s that air ambulances were realized. The future involves land, sea, and air operations for Emergency Medical Services, so Waterborne Coastal Ambulances should not be too wild of a dream.
Finally, I wish to inspire sweeping technological upgrades in EMS. A computerized radio system in which an Emergency Medical Responder’s call is indicated in a computer in his or her ambulance with turn-by-turn directions to the destination of that next call and the closed route to the adequate medical facility relevant to the patient’s needs. This should include global positioning systems in all land, sea, and air ambulances.
Shock-absorbing wheelchairs, stretchers, and hoya lifts should be available in each ambulance, and periodic physical and psychotherapy should be mandatory for Emergency Medical Responders. The moral of my story is I envision a future in which cultural awareness as it pertains to trendy subcultures in our community, tomorrow’s version of the modern upgrade of equipment, training, and duties, and mandatory periodic physical and psychotherapy will elevate Canada’s Emergency Medical Responders to world-class standards.*
REFERENCES
The context of this essay was drawn from the following websites:
1. Care Bear
Link: http://careerbear.com/paramedic/article/what-is-a-paramedic
Paragraph 1 (what is a paramedic)?
By Ylva Van Buuren
2. Ontario Paramedic Association (with direct quotations)
Link: https://www.ontarioparamedic.ca/paramedics/history-of-paramedics-and-ems/
Timelines: 1, 3, 6, 9, 23, 29, 29, 30 and 31
The author was not specified.
3. EMS1
Link: http://www.ems1.com/careers/articles/1058440-What-is-EMS-A-Definition/
Paragraph 3 (What is EMS: A Definition)
By EMS1 Contributors
4. The Conference Board of Canada
Link: http://www.conferenceboard.ca/cashc/research/2012/inconvenient_truths.aspx
Paragraphs 1, 2, 3 (The Inconvenient Truths about Canadian Health Care)
By Daniel Muzyka, Glen Hodgson, and Gabriela Prada.